What is an inguinal hernia?
An inguinal hernia occurs in the abdomen near the groin area. They develop when fatty or intestinal tissues push through a weakness in the abdominal wall near the right or left inguinal canal. Each inguinal canal resides at the base of the abdomen.
Both men and woman have inguinal canals. In men, the testes usually descend through their canal by around a few weeks before birth. In women, each canal is the location of passage for the round ligament of the uterus. If you have a hernia in or near this passageway, it results in a protruding bulge. It may be painful during movement.
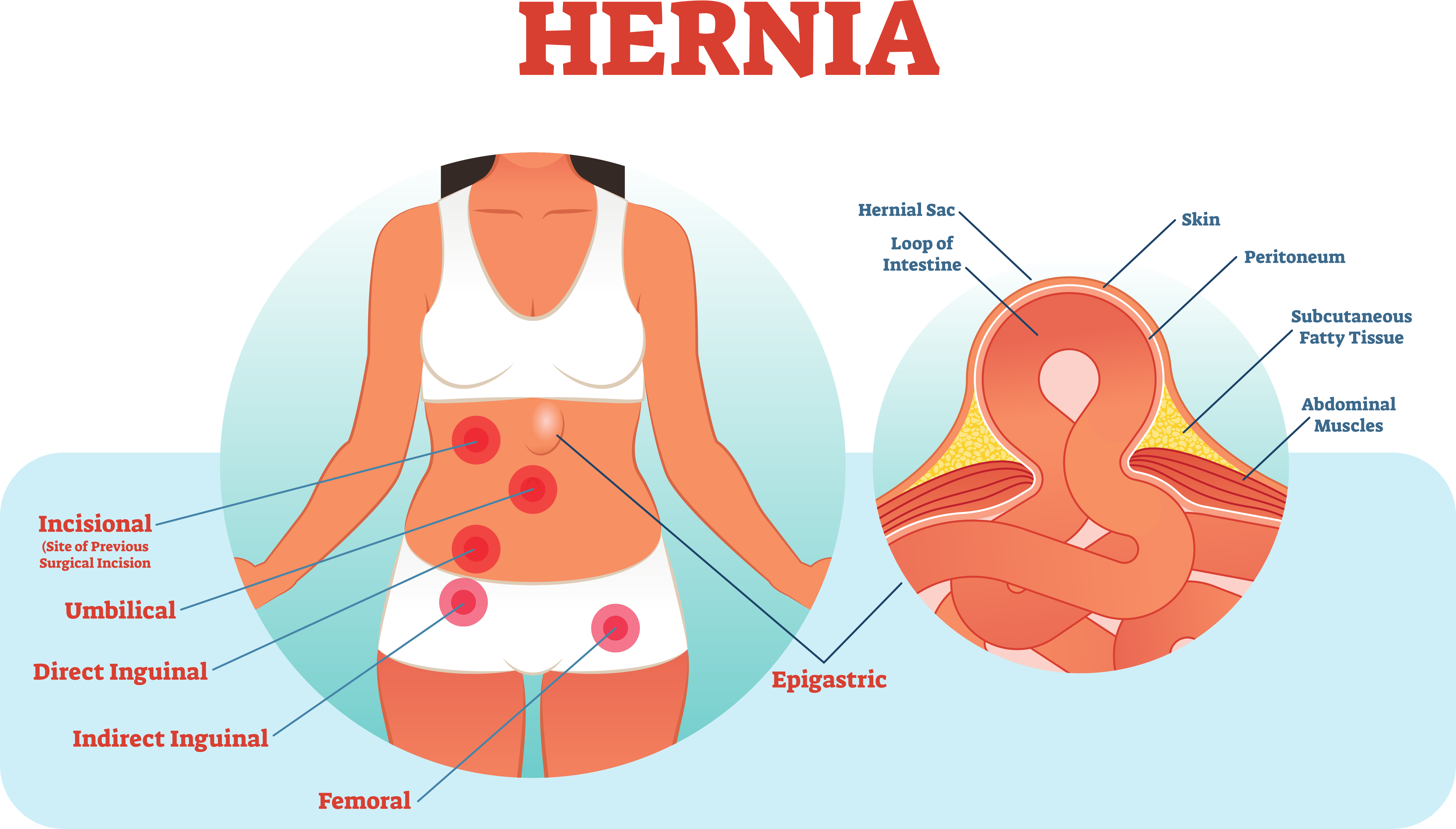
Many people don’t seek treatment for this type of hernia because it may be small or not cause any symptoms. Prompt medical treatment can help prevent further protrusion and discomfort.
Treating inguinal hernias
Surgery is the primary treatment for inguinal hernias. It’s a very common operation and a highly successful procedure when done by a well-trained surgeon.
Options include either an open inguinal herniorrhaphy or laparoscopic inguinal herniorrhaphy. In open inguinal herniorrhaphy, one larger incision is made over the abdomen near the groin. In laparoscopic inguinal herniorrhaphy, multiple smaller abdominal incisions are made. A long, thin tube with a lighted camera on the end helps the surgeon see inside your body to perform the surgery.
The goal of either surgical approach is returning the internal abdominal tissue(s) back into the abdominal cavity and repairing the abdominal wall defect. Mesh is commonly placed to reinforce the abdominal wall. Once structures are put into their proper place, your surgeon will close the opening with sutures, staples, or adhesive glue.
There are potential pros and cons to open inguinal hernia repair versus laparoscopic. For instance, laparoscopic herniorrhaphy may be preferable if you want a shorter recovery time. But your risk of hernia recurrence may be greater with laparoscopic repair.
Source: https://www.healthline.com/health/inguinal-hernia#treatment
